Alright future obstetricians, let’s walk through the incredible, sometimes unpredictable, but often beautiful journey of understanding normal labour. Specifically, we’ll dive deep into the stages of labour, the dynamic process involving the patient, the baby, and the skilled healthcare team guiding them. It’s not just about dilation and contractions; each phase presents unique challenges and requires specific management. We’ll follow the chronological path from the moment a pregnant woman arrives at the ward, through the distinct stages of labour, to the triumphant arrival of the baby and the equally important postpartum period. All crucial clinical details will remain in focus, and we’ll cite our sources [1, 2, 3].
Arrival and Assessment – Recognizing the Onset of Labour
Imagine this: a pregnant woman arrives at the labour ward, reporting contractions. Your first job? Figure out if this is really labour or just a practice run. Those pesky Braxton Hicks contractions can be misleading. This is where your initial assessment skills shine. You’ll gather clues to confirm the diagnosis and determine which of the stages of labour has begun [2].
Gathering the Patient’s Story
You’ll start with a focused history. Ask about when the contractions began. How often are they coming (frequency), how long do they last (duration) and how strong do they feel (intensity)? Furthermore, don’t forget to ask about any fluid leaks. Note when it happened, how much, and what colour it was. Any bleeding beyond just the little bit of “show,” which is the mucus plug, is also important to note [2].
Performing the Physical Examination
Following the history, you’ll move to the physical exam. Use abdominal palpation to feel those contractions yourself. Are they regular and getting stronger? This is also your chance to assess the baby’s position. Determine their lie, presentation, and position. Is the baby head-down? Where’s their back? In addition, you’ll get a rough idea of the baby’s size. Feel how much of the baby’s head is still sitting above the pelvic brim [2].
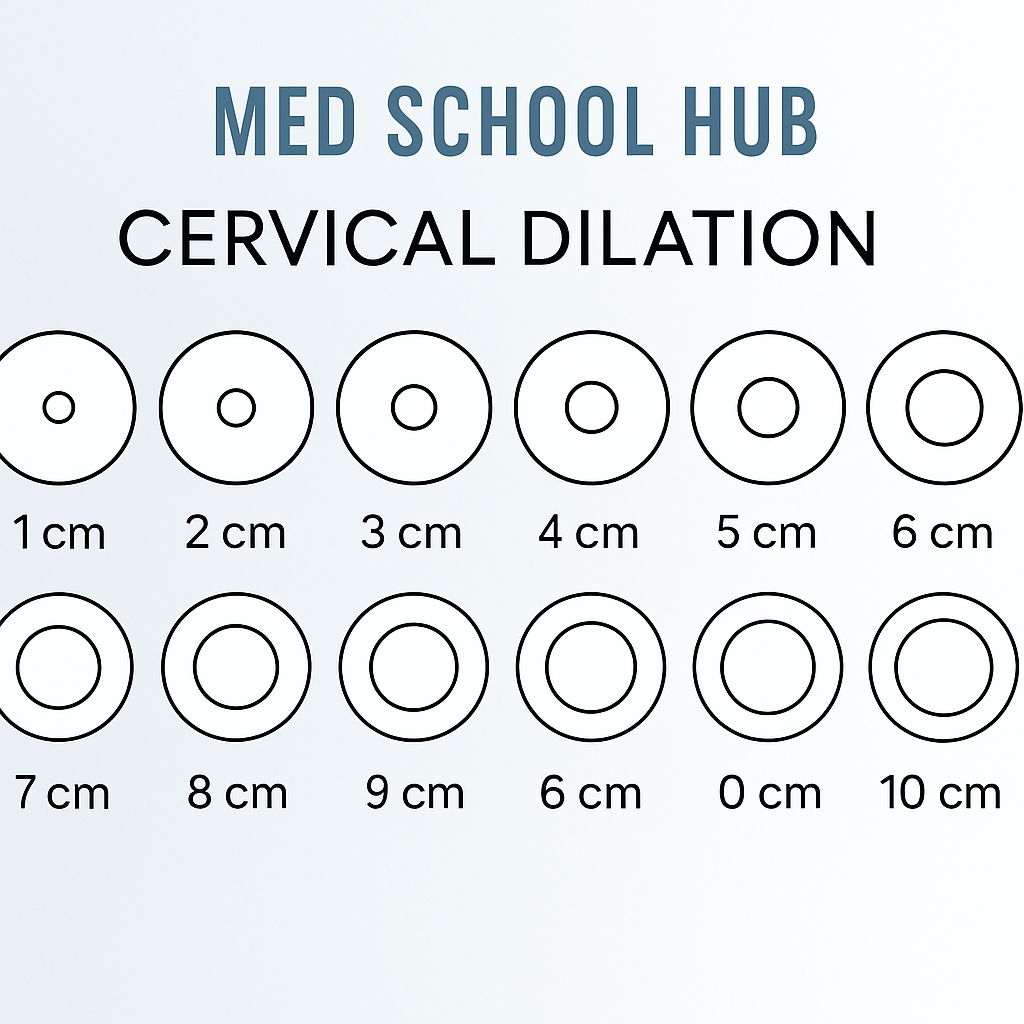
A sterile vaginal examination is a key part of assessing progress through the stages of labour. However, remember to only perform it when indicated. Minimize frequency, especially if the waters have broken, to reduce the risk of infection [2, 3]. During this exam, you’re checking several critical parameters: dilation, which is how open the cervix is, measured in centimeters from 0 to 10 cm; effacement, or how thin the cervix has become, measured in percentage from 0% (thick) to 100% (paper-thin); the cervix’s consistency (soft, medium, firm) and position (anterior, mid, posterior); and the baby’s station. Station tells you how far down the presenting part (usually the head) is in relation to the mother’s ischial spines. This is measured in centimeters, with 0 station being level with the spines, negative numbers meaning above, and positive numbers meaning below. As the baby descends, the station number increases [2]. You’ll also evaluate the status of the membranes. Are the amniotic membranes intact or ruptured? If ruptured, note the time and the colour of the amniotic fluid. Clear is good, but meconium-stained (greenish/brown) needs closer attention [2].
If the patient thinks her waters have broken but isn’t having regular contractions, a sterile speculum examination is often preferred over a digital vaginal exam. You can visualize the cervix and look for pooling amniotic fluid. This minimizes the increased infection risk of a digital exam in this scenario [2].
Confirming the Labour Diagnosis
You diagnose established labour when those regular, painful contractions are causing progressive cervical change. This means both effacement and dilation are occurring [2]. If you’re not sure whether it’s true labour, don’t guess! Re-examine after 2-4 hours to see if there’s been a change in the cervix [2]. Understanding the nuances here is key to identifying when labour deviates from the norm. Consequently, you can learn more about recognizing and managing Abnormal Labour in our dedicated article on the topic.
Navigating the First Stage of Labour
Okay, diagnosis confirmed! Welcome to the labour ward. The first stage is the longest of the stages of labour. Its main focus is on cervical dilation [1, 2]. Think of it as having two distinct acts: the latent phase and the active phase.
Scene 1: The Latent Phase (0-4 cm) – The Beginning of Dilation
In the latent phase, the cervix is effacing and slowly dilating up to about 4 cm. Contractions are often irregular, perhaps 5-20 minutes apart, and less intense. They feel more like strong period pain [1, 2]. This phase is the wildcard in terms of duration. It can last anywhere from hours to days, especially for first-time mothers [2].
Your role here is to keep the patient comfortable and supported. Encourage hydration. Oral fluids are great if there are no complications, but IV fluids like 100 mL/hour are also common. Good hydration helps contractions and reduces the risk of blood clots [2, 3]. Encourage mobility and position changes as the patient feels comfortable. Offer simple pain relief options: non-pharmacological methods like massage, warm baths or showers (hydrotherapy), relaxation techniques, or using a TENS machine. Similarly, simple oral analgesics like paracetamol or paracetamol with codeine can also be used here [3]. Patients might even stay in a lower-acuity area or go home if it’s safe and they prefer [3].
Scene 2: The Active Phase (4-10 cm) – Accelerating Dilation
Things really pick up in the active phase! The cervix is now dilating more rapidly, moving from 4 cm to the full 10 cm. Contractions become stronger, more regular (for example, every 3-5 minutes), and last longer [1, 2]. This phase typically lasts 4-8 hours or more, with an average dilation rate of about 1 cm per hour in first labours [2].
Monitoring and Pain Management in the Active Phase
Your role shifts to closer monitoring and active support during this crucial part of the stages of labour. You’ll keep a close eye on both mum and baby. Monitor maternal vital signs like blood pressure, pulse, and temperature. Assess contractions by palpation or using a cardiotocograph (CTG) [2, 3]. Crucially, you’ll monitor the baby’s heart rate (FHR). This can be done either intermittently with a Pinard stethoscope or Doppler, or continuously with a CTG, especially if there are risk factors or interventions like an epidural or oxytocin augmentation [2, 3]. Learning to interpret those CTG traces is vital. Understand the baseline FHR, variability, accelerations, and decelerations; this is your language here [3].
Chart everything on a partogram. It’s a visual roadmap of labour progress that helps you spot potential problems early [2]. This essential tool allows you to track cervical dilation, fetal descent, contraction patterns, and maternal and fetal well-being over time. For a deeper dive into using and interpreting the partogram, check out our article specifically on the Partogram.
Pain often ramps up significantly in this phase, so offer stronger options. Inhaled analgesia like Nitrous Oxide and Oxygen is patient-controlled and works quickly during contractions. Injected Opioids such as Pethidine, Morphine, or Remifentanil (given intravenously via a patient-controlled pump) provide systemic relief. However, be mindful of potential maternal sedation and neonatal respiratory effects if given close to birth [3].
The gold standard for pain relief in labour is often Epidural Analgesia. An anesthetist places the epidural catheter in the epidural space to provide continuous local anesthetic, often combined with an opioid. It’s very effective but requires monitoring for hypotension and often a urinary catheter [3]. It’s worth noting that while epidurals don’t increase C-section rates, they can sometimes prolong the second stage and might increase the likelihood of needing an instrumental delivery [3]. Spinal blocks are typically used for rapid, short-acting anesthesia, often for instrumental deliveries or Cesarean sections [3].
General Care During the First Stage
Continue encouraging position changes and mobility if possible. Maintain hydration. Minimize vaginal exams to check progress, balancing the need for information with the risk of infection [2, 3].
The Grand Finale – The Second Stage of Labour: Birth!
The grand finale begins when the cervix is fully dilated at 10 cm! This marks the start of the second of the stages of labour, which ends with the birth of the baby [1, 2]. The patient might feel an overwhelming urge to push as the baby descends through the birth canal [1, 2].
The duration of this stage can vary, from as quick as 30 minutes to a few hours. It can potentially last up to 3 hours (or 4 hours with an epidural) in first labours, and usually shorter in subsequent labours [2, 3]. The second stage is often divided into a passive phase of descent and rotation, followed by an active phase of maternal expulsive efforts [1].
Your role is to coach and support the patient’s pushing efforts. Continue monitoring the baby’s well-being, often with continuous FHR monitoring [2, 3]. As the baby’s head becomes visible at the vaginal opening, known as “crowning,” you’ll guide the delivery carefully. During vaginal exams in this stage, you’ll assess for molding, the temporary overlapping of the fetal skull bones to adapt to the maternal pelvis, and caput succedaneum, a localized swelling on the baby’s scalp caused by pressure. These are common findings and usually resolve after birth [2]. Once the head is born, you’ll observe restitution. This is where the head externally rotates to align with the baby’s shoulders, preparing for the delivery of the rest of the body [1].
The Aftermath – The Third Stage of Labour: Placenta and Recovery
The baby is out – truly amazing! But you’re not quite done yet. The third stage of labour is the delivery of the placenta [1, 2]. Mild contractions resume to help the placenta separate from the uterine wall. This stage is usually over in a few minutes, definitely within 30 [2].
Your role is crucial here with active management! Administer a uterotonic like Oxytocin right after birth to help the uterus contract down firmly [2, 3]. Watch for signs the placenta is separating, such as a gush of blood or lengthening of the umbilical cord. Use controlled cord traction to help deliver the placenta [2, 3]. Once it’s out, examine it carefully to ensure it’s complete. Massage the uterus afterwards to keep it firm and reduce bleeding [2, 3]. This active management dramatically lowers the risk of postpartum hemorrhage [3].
Immediately postpartum, you’ll check for any vaginal or perineal tears and repair them. Monitor maternal vital signs and vaginal bleeding closely. Encourage skin-to-skin contact with the baby and early breastfeeding. These are great for bonding and also help the uterus contract [3].
Heading Home – Discharge
Once mother and baby are stable, vital signs are normal, bleeding is controlled, and initial recovery is progressing well, preparations for discharge begin. Ensure the patient is comfortable. Make sure she understands postpartum care, including wound care if needed, monitoring bleeding, and recognizing signs of infection. Provide necessary follow-up appointments. Offer information on breastfeeding support and newborn care before they head home.
Glossary of Labour Terms
Remember these terms when assessing labour progress and observing the birth process within the stages of labour [1, 2]:
- Effacement: The thinning and shortening of the cervix, measured in percentage (0% to 100%). Think of it like the cervix getting “taken up” into the lower part of the uterus.
- Dilation: The opening of the internal cervical os, measured in centimeters (0 cm to 10 cm). This is the target!
- Station: The level of the fetal presenting part (usually head) relative to the maternal ischial spines. Measured in cm (-5 to +5, with 0 at the spines). It tells you how far down the baby has descended.
- Descent: The overall downward movement of the fetal presenting part through the pelvis.
- Position: The orientation of a landmark on the fetal presenting part (like the back of the head – occiput) relative to the mother’s pelvis (e.g., Occiput Anterior – facing forwards, most common and favourable).
- Molding: The temporary overlapping of the fetal skull bones during labour to adapt to the maternal pelvis. Common and usually resolves after birth.
- Caput Succedaneum: A localized swelling on the baby’s scalp caused by pressure during labour. Feels soft and boggy, also usually resolves.
- Restitution: The external rotation of the fetal head after it has emerged from the vagina, allowing it to align with the baby’s shoulders before the rest of the body is born.
References
- Baker PN, Kenny LC, editors. Obstetrics by Ten Teachers. 20th ed. CRC Press; 2017.
- Information from provided video transcripts [Internet]. [cited 2025 Apr 28]. Available from: Https://youtu.be/wApjq7cwBUc?si=5HghLf6zbPfI7SAt, https://youtu.be/nvspTAA_reg?si=cygwRzUxKM8FlhPb
- National Institute for Health and Care Excellence (NICE). Intrapartum care for healthy women and babies: Clinical guideline [CG190]. NICE; 2014 Dec [updated 2017 Feb; cited 2025 Apr 28]. Available from: https://www.nice.org.uk/guidance/cg190
.
You can try the MCQs on Normal and Abnormal Labour to revise this topic



Leave a Reply